Researchers from the University of Pennsylvania Perelman School of Medicine have discovered new ways to reduce inflammatory side effects of RNA therapies. Findings from the study, “Limiting Endosomal Damage Sensing Reduces Inflammation Triggered by Lipid Nanoparticle Endosomal Escape,” were published in Nature Nanotechnology.
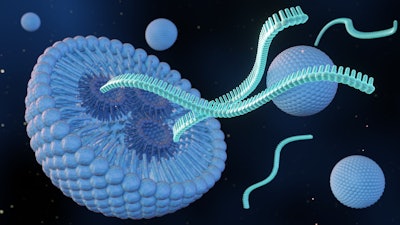
Lipid nanoparticles (LNPs) are a novel mechanism that can deliver medicines, genes and RNA to patients. The small fat bubbles enter cells using endosomes, tiny sacs that help direct materials to the right place. In some cases, LNPs delivering RNA can cause harmful inflammation if the endosomes burst and set off an immune response that triggers galectin.
The research team found two new solutions that allow RNA to still reach the desired endpoint while avoiding adverse inflammation. The first solution is to add a unique biodegradable fat molecule, called 4A3-SC8, to the LNP, which can repair the endosome to lessen the impact of a burst. The second is to add a drug called thiodigalactoside (TG), which blocks inflammation. TG is commonly used to treat inflammation and cancer.
“This [discovery] represents meaningful progress for RNA-based therapeutics,” said Serena Omo-Lamai, first author and PhD student researcher, in a university news release. “Our approaches could make LNPs safer and more versatile, opening doors to treat inflammatory diseases that were previously out of reach.
Scientists tested the strategies in mouse models that had acute respiratory distress syndrome (ARDS) and found both to be effective and safe, successfully reducing lung inflammation and tissue damage while delivering the mRNA therapy to treat ARDS.
“By designing LNPs that cause less damage and block inflammation pathways, we can expand RNA treatments to conditions like ARDS, heart attack and stroke, where inflammation is a major challenge," said study co-author Jacob Brenner, MD, PhD, assistant professor of pulmonary, allergy and critical care.
Dr. Brenner clarified that mRNA drug delivery used in vaccines, like the one for COVID-19, operates differently and does not fall into this category of LNPs that pose inflammatory risk.
“Vaccines rely on LNPs to stimulate the immune system throughout the body, which is key to their success, but this immune activation can worsen conditions like stroke or ARDS when LNPs are used as treatments,” he said. “Our study shows how to make LNPs safer for such diseases by reducing unwanted inflammation.”